Imagine planning your long road trips, sharing your weekend vibes with your family, without worrying about any bloating, nausea, or indigestion. A life without any stomach issues is not a dream – a reality that everyone desires. Suddenly, your stomach goes back, steals your healthy gut, and you feel crampy pain inside, digestive disorders, which could be a concerning matter. Your digestion, everything slows down—your energy, your appetite, and even your daily living.
In the early stages, gastroparesis may remain silent. Many people rely on medications to manage occasional symptoms. But if the warning signs are ignored, the condition may worsen and lead to several digestive problems such as acid reflux, bloating, gastritis, and persistent stomach pain.
Gastroparesis occurs when the stomach’s nerves and muscles cannot properly process food. This condition can cause significant discomfort and digestive disturbances, often requiring medical attention for proper management.
What is gastroparesis, and how does it affect digestion?
Gastroparesis is often referred to as “stomach paralysis.” In this condition, the stomach cannot effectively move food into the small intestine for digestion.
Normally, stomach muscles contract to push food through the digestive tract. In gastroparesis, these muscles and the stomach nerve are damaged, preventing the stomach from emptying properly. As a result, food remains in the stomach longer than normal.
Patients often experience uncomfortable digestive symptoms that may lead to long-term complications. These complications can include loss of appetite, difficulty meeting nutritional needs, and unstable blood sugar levels.
When food stays in the stomach for too long, it may partially harden into a solid mass known as a bezoar, which can block the digestive tract.
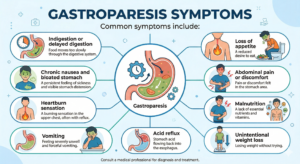
Gastroparesis symptoms:
Symptoms of gastroparesis after eating are mainly caused by food remaining in the stomach for an extended period without proper digestion.
Common symptoms include:
- Indigestion or delayed digestion
- Chronic nausea and bloated stomach
- Heartburn sensation
- Vomiting
- Acid reflux
- Loss of appetite
- Abdominal pain or discomfort
- Malnutrition
- Unintentional weight loss
Types of Gastroparesis:
Although it is not usually life-threatening, it can occur in different forms depending on its underlying cause.
-
Diabetes-Related Gastroparesis:
When diabetes damages the nerves that control stomach muscles, food cannot move normally into the small intestine. This condition is known as diabetic gastroparesis.
-
Post-Surgical Gastroparesis:
Gastroparesis may develop after surgery involving the stomach or nearby organs. Nerve damage during surgery can slow down stomach emptying.
-
Idiopathic Gastroparesis:
In many cases, the exact cause of gastroparesis cannot be identified. This form is known as idiopathic gastroparesis.
Gastroparesis causes:
It typically occurs when the vagus nerve, which controls stomach muscle contractions, becomes damaged. Here, you get what causes gastroparesis in adults, including
Diabetes causes gastroparesis:
Long-term uncontrolled diabetes can damage the vagus nerve. When this nerve is affected, food movement through the digestive tract slows down or stops.
Stomach nerve damage (Vagus Nerve Dysfunction):
The vagus nerve controls stomach muscle contractions. Damage can occur due to:
- Surgery involving the stomach or the oesophagus
- Neurological disorders
- Trauma
Surgery
Any surgery near the stomach can sometimes lead to gastroparesis due to nerve damage.
Viral Infections
Certain viral infections may temporarily disrupt the nerves controlling stomach movement.
Medications
Some medications can slow stomach emptying by affecting stomach nerves and muscles.
Endocrine Disorders
Hormonal imbalances and endocrine conditions—such as thyroid disorders, adrenal problems, electrolyte imbalance, or kidney disease—may interfere with nerve signalling and digestion.
Neurological Disorders
Conditions affecting the nervous system, such as Parkinson’s disease, multiple sclerosis, or autonomic nervous system disorders, may disrupt stomach nerve function.
Cystic Fibrosis
In people with cystic fibrosis, thick mucus may accumulate in the digestive tract and slow stomach movement.
Autoimmune Diseases
In autoimmune conditions, the immune system mistakenly attacks the body’s own cells. Some studies suggest that antibodies may damage the nerves controlling the stomach, contributing to gastroparesis.
How do you feel if you have gastroparesis?
During this condition, your stomach muscles are not working or moving, so what you have eaten is not going to pass, and it stays in your stomach for a long time, which means delayed gastric emptying. In this condition, you feel immediately full after eating. You may feel sudden stomach pain, cramping, upper abdominal discomfort, and feeling nauseous. You also feel, in some cases, heartburn if your stomach produces excess acid.
Risk Factors of Gastroparesis
It is often linked to other health conditions that affect the nervous system or digestion.
Uncontrolled Diabetes
Delayed stomach emptying can disrupt how glucose enters the bloodstream. Blood sugar levels may fluctuate unpredictably, causing complications for people with diabetes.
Neurological Disorders
Conditions affecting the nervous system may interfere with stomach nerve signals and digestion.
Bezoar and Gastric Outlet Obstruction
Undigested food may harden into a mass called a bezoar. If it grows large enough, it can block the stomach’s exit and prevent food from entering the intestines, causing a gastric motility disorder.
- Autoimmune diseases:
Autoimmune conditions can damage the nerves that control stomach muscle contractions. This disrupts normal digestion and slows the movement of food from the stomach. - Abdominal distension:
Persistent abdominal distension indicates delayed stomach emptying and gas buildup. It reflects impaired gastric motility and increased digestive dysfunction. - Obesity:
Obesity is linked to metabolic and nerve-related changes that affect stomach function. These changes can slow gastric emptying and increase the risk. - Weight loss:
Unintentional weight loss occurs when delayed digestion or digestive disorders reduce appetite and nutrient absorption. Over time, poor stomach emptying leads to inadequate nutritional intake and body weight decline.
Does Gastroparesis affect your bowel movement (poop)?
During this condition, you experience slow stomach emptying, which affects your bowel movement, such as constipation and delayed bowel movement. This condition may vary in people and their condition of gastroparesis. As foods are not even digested well, some pieces are directly sent to the intestines, which causes difficulty with smooth bowel movement.
Constipation or delayed bowel movements.
Food that is not fully digested in the stomach may pass unevenly into the intestines, which can disrupt normal bowel movement patterns.
Gastroparesis diet plan for patients:
Although with various suggestions, diet is a crucial part of reducing any stomach disorders. There is no specific remedy along with a diet change for gastroparesis management.
But you may be conscious about your diet chart to reduce the complications of gastroparesis and instigate smoother digestion.
- Eating smaller and more frequent meals may reduce your intense bloated feeling.
- Try to consume low-fat and fibre-rich foods to avoid slow digestion.
- Avoid drinking soda and alcohol, which are other primary causes of gastroparesis
- Make sure your body gets enough nutrition and hydration as it needs.
- Have some light exercises like walking, yoga, that increase your mobility and help with digestion
- Maintaining stable blood glucose improves gastric function.
Foods to Avoid with Gastroparesis:
- High-Fat Foods: Fried foods, oily snacks, fatty meats, and heavy dairy products should be limited because fat slows stomach emptying and may worsen delayed digestion, especially in people suffering from a stomach motility problem.
- High-Fibre Foods: Raw vegetables, broccoli, cabbage, beans, lentils, and whole grains can be difficult to break down. These foods may stay longer in the stomach and aggravate a gastrointestinal motility disorder.
- Nuts, Seeds, and Tough Fruit Skins: Foods like peanuts, sunflower seeds, pumpkin seeds, and fruits with thick skins can accumulate in the stomach and make stomach digestion problems more uncomfortable.
- Carbonated Drinks: Fizzy beverages and sodas can increase bloating and gastric pressure, which may worsen symptoms of a chronic digestive disorder like gastroparesis.
- Processed and Heavy Foods: Fast foods, packaged snacks, and overly rich meals are harder to digest and can intensify delayed digestion in individuals dealing with a gastrointestinal motility disorder.
- Alcohol and Excess Caffeine: These can irritate the digestive tract and interfere with normal stomach function, potentially worsening a stomach motility problem and other chronic digestive disorders.
Gastroparesis treatment options:
What you need to know is the best treatment for gastroparesis. Though there is no specific process by which you can reduce its risks. Medications are the primary treatment options for curing gastroparesis, as suggested by your doctor.
Medications
Doctors often prescribe medications that stimulate stomach muscle movement or help relieve nausea and vomiting.
Gastroparesis diagnosis:
Doctors may recommend tests to diagnose gastroparesis or rule out other digestive conditions.
Tests used to diagnose gastroparesis:
Blood tests help detect nutritional deficiencies, infections, or metabolic issues. Get in touch with Nirnayan Healthcare, a trusted laboratory chain across Kolkata, offering comprehensive blood tests and diagnostic services for early and accurate disease detection.
Ultrasound
Ultrasound imaging helps identify structural problems involving organs such as the gallbladder or kidneys.
Upper Gastrointestinal (GI) Endoscopy
This procedure allows doctors to examine the oesophagus, stomach, and the upper part of the small intestine.
Breath Tests
Breath tests measure how quickly the stomach empties by tracking substances released during digestion.
Treatment for Severe Cases:
In more serious cases, advanced treatments may include:
- Gastric electrical stimulation
- Feeding tubes for nutritional support
- Surgical procedures, when necessary
When to See a Doctor:
You should seek medical advice if you experience:
- Persistent vomiting
- Rapid or unexplained weight loss
- Severe bloating
- Digestive symptoms along with uncontrolled diabetes
Early diagnosis and treatment can help prevent complications and improve quality of life.
Conclusion:
Gastroparesis can significantly affect daily life, but proper treatment, dietary adjustments, and lifestyle changes can help manage the condition effectively. If you experience ongoing symptoms such as persistent stomach discomfort, chest burning, or digestive issues, it is important to consult a healthcare professional. Early diagnosis and proper treatment can help improve digestion and overall well-being.
Regular health check-ups and diagnostic tests can also help detect underlying conditions early and support better digestive health.